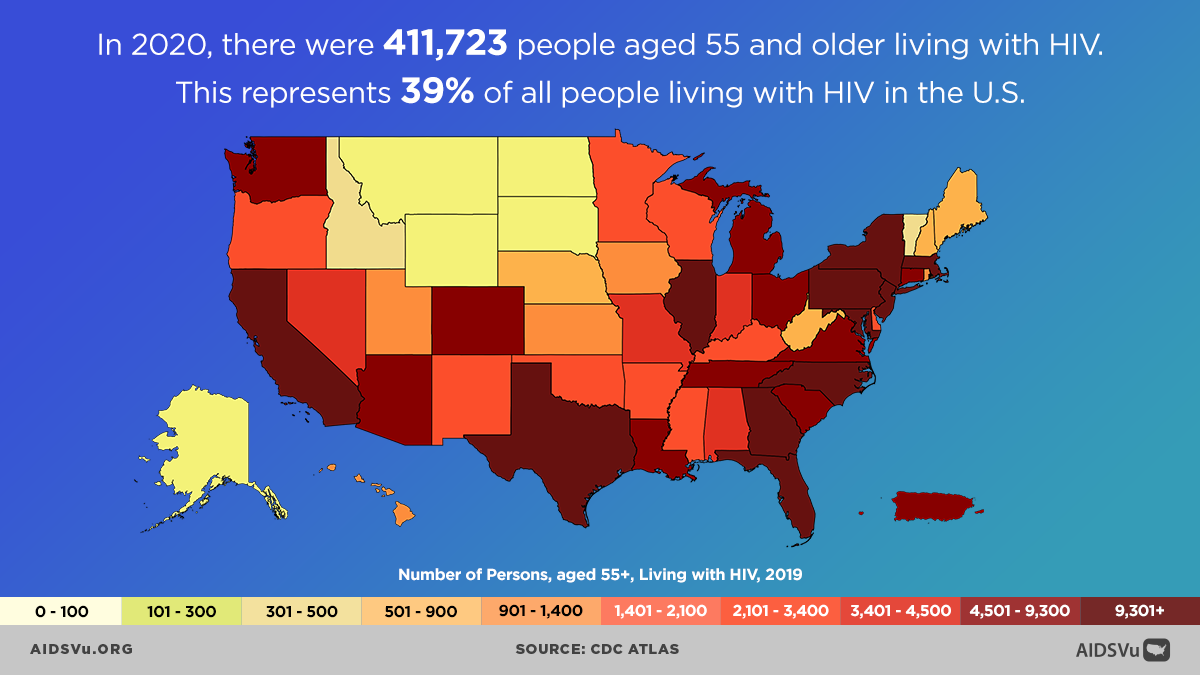
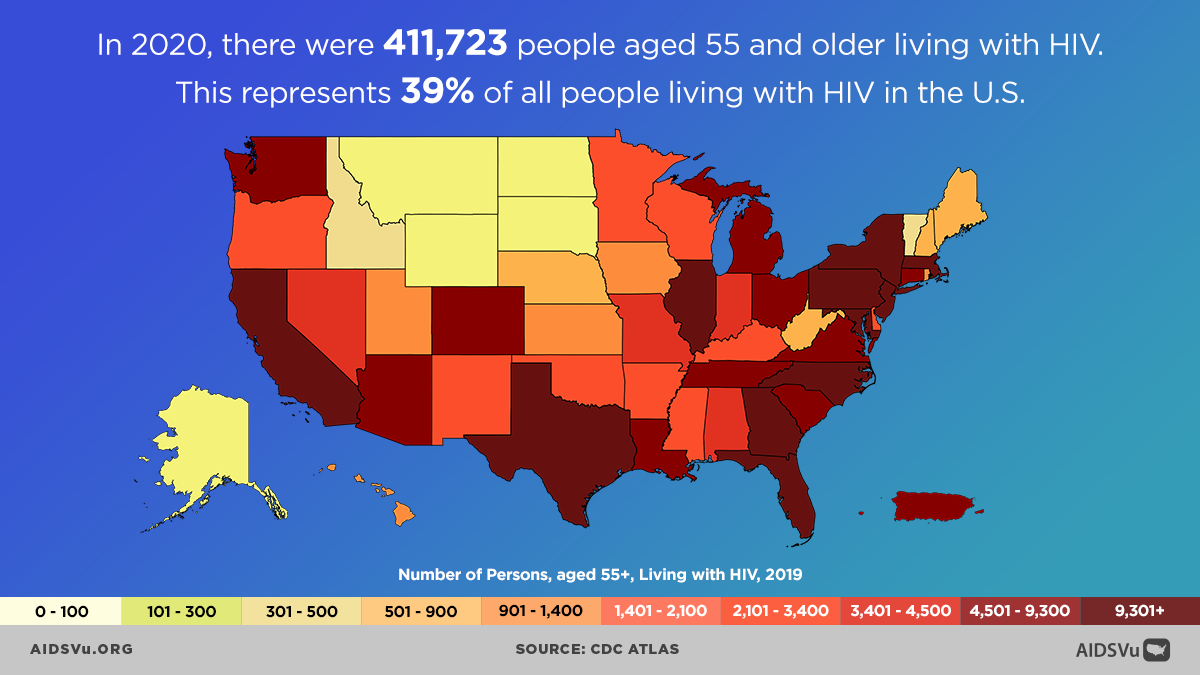
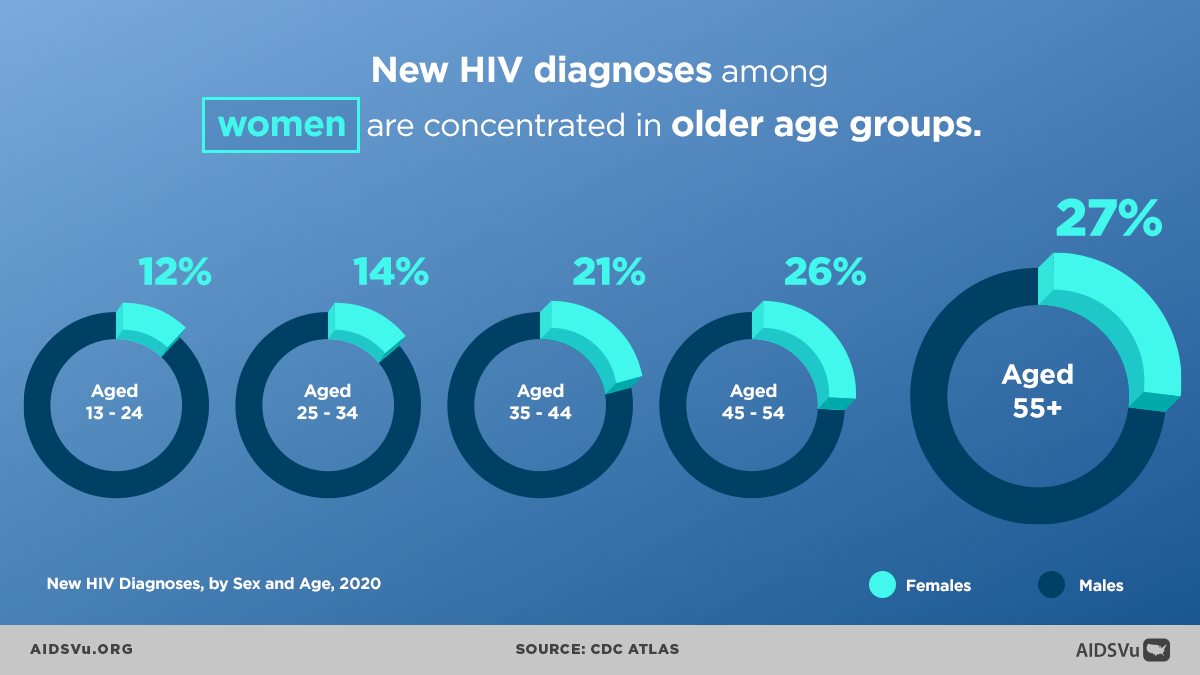
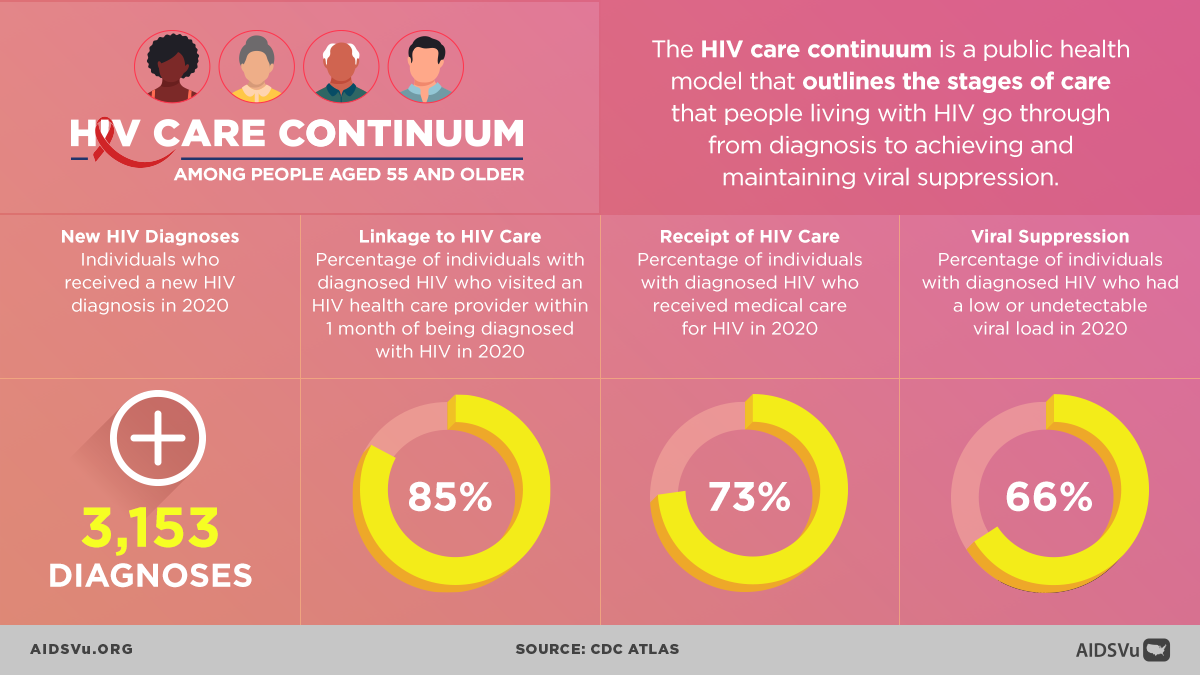
In 2020, there were 411,723 people aged 55 and older living with HIV, representing 39% of the U.S. population living with HIV. In the same year, out of all people newly diagnosed with HIV, 10% were aged 55 and older. Additionally, for people 55 and older living with diagnosed HIV:
- 85% were linked to care;
- 73% received care;
- 66% were virally suppressed – the highest viral suppression rate out of all age groups.
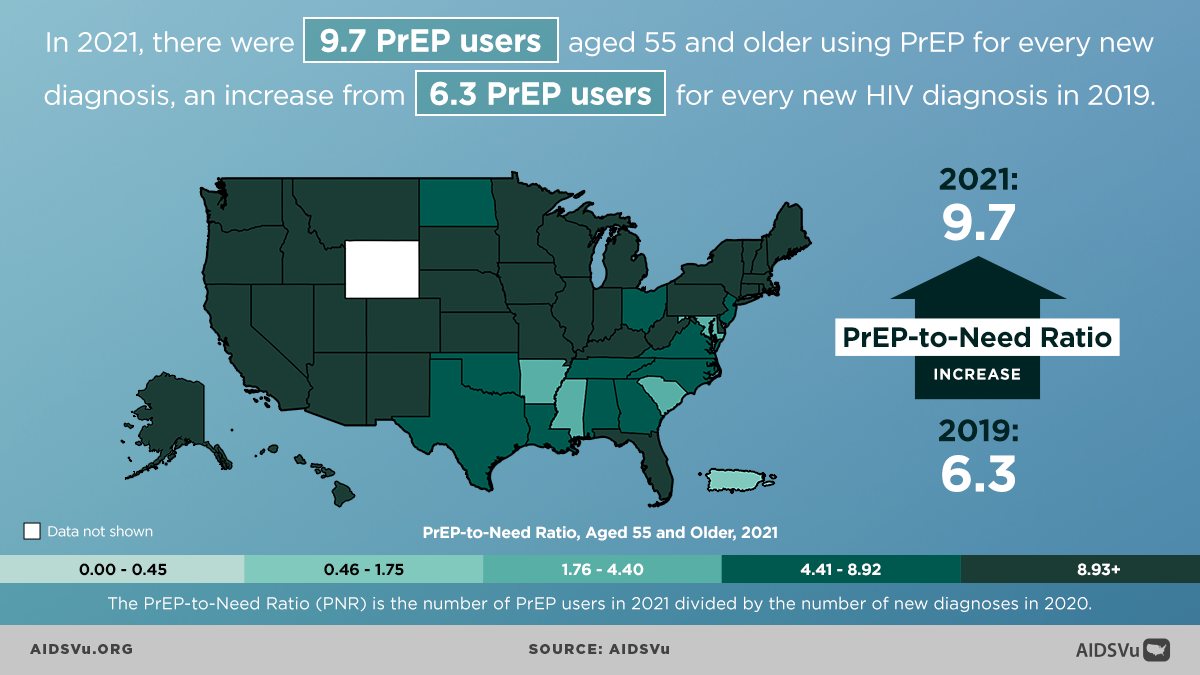
From 2020 to 20121, there was a 23% increase in the number of PrEP users among this age group. The PrEP-to-Need Ratio, which is the number of PrEP users divided by the number of HIV new diagnoses, has also increased, with 9.7 PrEP users aged 55 and older using PrEP for every new diagnosis in 2021 compared to 6.3 PrEP users for every new HIV diagnosis in 2019, indicating a lower unmet need for PrEP.
Older adults living with HIV face additional aging-related challenges with multiple chronic conditions like cardiovascular disease, lung disease, obesity, and more. Stigma stemming from isolation due to a lack of social support and/or illness may also prevent older individuals from accessing HIV-related health care or disclosing their HIV status.
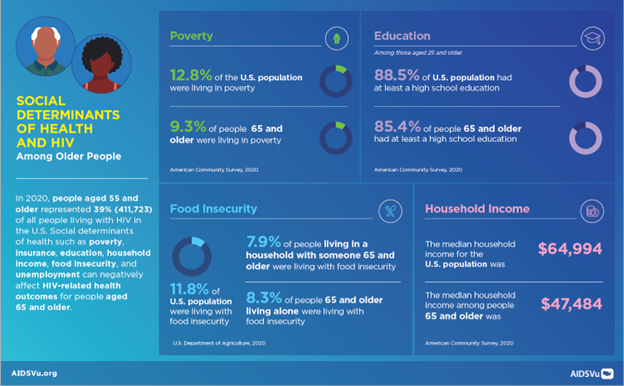
In addition to aging-related challenges, racial disparities and social determinants of health such as poverty, insurance status, education, household income, food insecurity, and unemployment can negatively impact HIV-related health outcomes for this age group. For example:
- Black Americans 55 and older had the highest number of new HIV diagnoses (1,241 diagnoses) and deaths among people living with HIV (4,818 deaths) compared to other races/ethnicities in the same age group
- In 2020, Americans 65 and over had a far lower median household income ($47,000) than the national average of $65,000